What is type 2 diabetes?
In a human body, all the cells get energy required for their processes through glucose. The food we eat, as it gets digested, is broken down to nutrients and most importantly, glucose and released into blood. When a person’s pancreas is unable to produce enough insulin to regulate normal sugar levels in the blood or is present but the body cannot utilize insulin properly, the condition is termed as Type 2 diabetes.
The condition usually develops slowly over years and so the symptoms may not be noticeable. Before diabetes develops, these people may have slightly higher values than normal but not very high to confirm diabetes, which is pre-diabetes – at this stage, making even slight changes in the lifestyle can help you prevent developing type 2 diabetes.
Unlike type 1 diabetes which majorly affects young age groups, type 2 diabetes is more prevalent in people of middle-age or older age populations and accounts for about 85-95% of the total diabetic population. The condition is mostly seen in people who are overweight or obese and are physically inactive. It could also be seen in elderly people who may not be overweight.
The most common, widely studied cause of type 2 diabetes is insulin resistance which is a Type 2 Diabetescondition that decreases the body cells response to insulin, thereby raising the blood sugar levels. A common feature of a person having insulin resistance is the presence of a darkened velvety skin on the neck and armpits. Being overweight and physically inactive are two strongly associated modifiable factors that could increase the likelihood of developing insulin resistance. In such people, excess belly fat in the body produces certain hormones in the body which promote insulin resistance. In addition, they can also contribute the risk for other heart and blood vessel related disease.
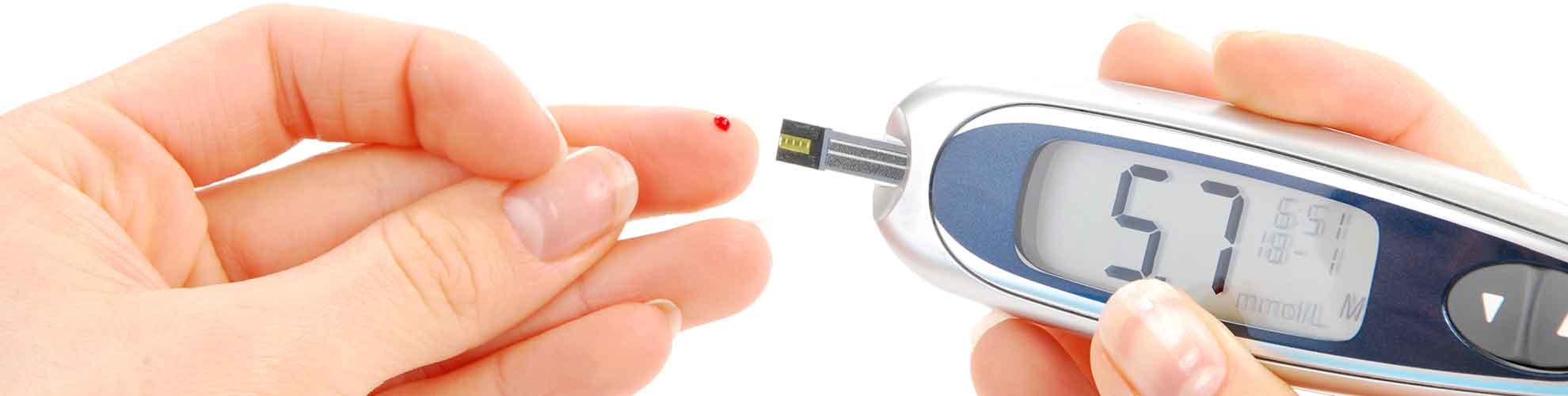
Therefore, treatment and prevention strategies for type 2 diabetes primarily focus on lifestyle interventions such as a balanced diet and regular activity that can not only reduce significantly the risk but also sometimes reverse the condition. Hence, not only medicines but also diet and exercise play a key role in diabetes management. In addition to these pillars, self-monitoring of blood glucose is another key component of diabetes management which helps you to track and achieve better sugar control.
Although diabetes doesn’t produce any life-threatening symptoms in a short term, it can significantly deteriorate the health by leading to serious health complications that may result in blindness, kidney failure, heart attack, amputation of legs. Primary reason for such complications is the presence of high sugar levels over long periods that cause changes at a micro level in your body and impair the functionalities. So, special care and attention to diabetes complications through regular screening and appropriate management and preventions strategies measures is necessary.
Type 2 Diabetes Causes & Risk Factors
Type 2 diabetes is a chronic condition in which either insulin levels become too low than necessary level to maintain a normal blood sugar level or body cells cannot respond to insulin and do not absorb glucose. Both the above phenomena lead to rise in the blood sugar levels. Multiple factors can influence the development of type 2 diabetes – especially genetic and environmental. Exact reasons for type 2 diabetes development are less understood, but there has been evidence showing some common factors that are likely to increase risk for type 2 diabetes. These are:
A person can have higher chances of becoming type 2 diabetic, if any or more of the close family members have it. The reason is that genetic susceptibility of an individual is strongly correlated with the condition because the genes responsible for protecting or predisposing a person to diabetes are carried genetically from the family members. A chart showing the chances of a person’s risk for developing type 2 diabetes depending on the family history.
Apart from the genetic factors, some modifiable risk factors like physical inactivity and obesity are also strongly associated risk factors for type 2 diabetes. When a person adapts a sedentary lifestyle or doesn’t engage in regular physical activity, or gains more weight with a high body mass index (BMI), the person may eventually develop insulin resistance. Particularly, excess belly fat is the primary cause of insulin resistance. The term refers to a state where the body becomes less responsive to insulin, especially, muscle, liver and fat tissues. The cells gradually lose their ability to absorb glucose, thus retaining more sugar in blood itself. To maintain a normal sugar level, compensating the sugar, pancreas produces high amounts of insulin. But due to many factors, production of insulin decreases, leading to the conditions pre-diabetes and diabetes.
What are the symptoms of type 2 diabetes?
Symptoms of diabetes are more likely to be noticeable with type 1 diabetes while the early symptoms can be missing in type 2 diabetes. This difference is due to the rapid onset and progression of symptoms with type 1 diabetes, and with type 2, they develop slowly over years, which are often mild and most of the type 2 diabetics could not feel any symptoms.
Typically, both forms of diabetes, type 1 and type 2 result in common symptoms such as:
- Increased appetite – although the blood sugars are high, the cells cannot take this glucose and this lack of energy makes a person feel hungry
- Increased thirst
- Frequent urination – occurs because the excess sugar leaks into urine through the kidneys and pulls extra water along dehydrating your body
- Fatigue – feeling very tired
- Headache
- Irritability
- Weight loss
- Itching or infections around the genital areas of men and women
- Slow healing of cuts or wounds
- Blurred vision due to dryness of eye lens
Another symptom specific to type 2 diabetes is darkening of skin at certain areas like neck, armpits, that is a sign of insulin resistance (reduced responsiveness)
If the early symptoms of either diabetes type 1 or type 2 are not evaluated and not managed appropriately, at later stages, the blood sugar levels rise very high and result in acute episodes requiring emergency treatment. During these episodes, along with typical diabetes symptoms like urination, increased thirst, additional visible symptoms could be fruity breath, troubled breathing, vomiting, increased heart rate, weakness, stomach pain, loss or altered consciousness, sometimes seizures or other neurological problems.
Therefore, all people at risk of type 2 diabetes should get checked for the condition and complications despite the presence or absence of the symptoms.
Treating Type 2 Diabetes
If people with type 2 diabetes are not diagnosed in time, they will have long periods of high blood sugar that causes damage to various body parts. In fact, people already show evidence of complications of heart, nerve, kidney, eye etc. even at the time of the first diagnosis of diabetes. Therefore, all people at risk of type 2 diabetes should get checked, even if they feel that they cannot spot any symptoms clearly.
What are the treatments of type 2 diabetes?
Diabetes is very common these days but that doesn’t meant that every individual has the same diabetes treatment plan. We highly encourage diabetics and their families to learn about latest therapies, treatment and approaches, as well as healthy lifestyle choices. This is where good communication with your diabetes experts come into play.
No treatment can completely cure diabetes, but the impact of the disease on overall health and complications can be reduced by bringing the sugar level close to normal through:
- Maintaining healthy diet
- Staying physically active through regular exercise
- Approximately 150 min of exercise per week such as walking, jogging, bike riding, skipping, swimming, etc. Another alternative is 75 minutes of vigorous intensity exercises each week, but only after your doctor has affirmed that your body can take that intensity.
- Taking anti-diabetic medications regularly as suggested by your doctor
- Unlike type 1 diabetes, where insulin is the main stay of treatment, various treatment options including insulin and also oral anti-diabetic drugs are available for managing type 2 diabetes
- Depending on various conditions such as comorbidities and complications, and risk of hypoglycaemia, weight consideration, your doctor may put you on the best possible treatment
- Monitoring the sugar levels regularly
- Taking medicines for managing the complications of the eye, kidney and heart
- Prevention of foot problems by taking good care of your feet
- Quitting smoking and reducing the alcohol intake which have significant impact on the complications
- Maintaining lipid levels and blood pressure under control
Monitoring your diabetes treatment
Following all the steps recommended by your doctor in your diabetes management is a must but what’s equally important is monitoring that treatment in a diabetes centre. This will indicate whether the current treatment is bearing fruit or alterations to your regime are required. For example, your blood sugar may be well controlled by lifestyle measures alone for a number of years but in time, you may need to add in one tablet. Later, you may need another. The only way to understand these requirements is by regular monitoring at our diabetes centre.
| BLOOD LIPIDS | BLOOD PRESSURE |
|---|---|
| Target: High Density Cholesterol: Men >40 mg/dL; Women >50 mg/dL Low Density Cholesterol: Very low Density Cholesterol: (as discussed with your physician) |
Target: 130/80 mm/Hg or less (as discussed with your physician) |